Medication Reconciliation Audit Tool Template - Discharge
ADVERTISEMENT
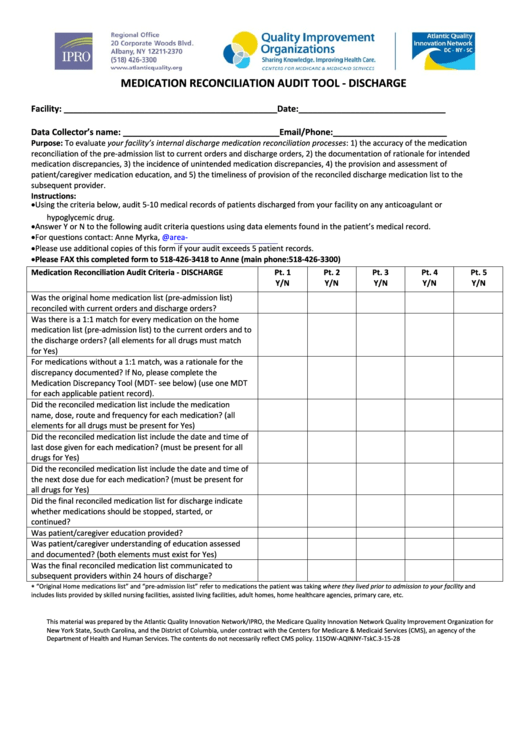
MEDICATION RECONCILIATION AUDIT TOOL ‐ DISCHARGE
Facility: _____________________________________________Date:_______________________________
Data Collector’s name: _________________________________Email/Phone:________________________
Purpose: To evaluate your facility’s internal discharge medication reconciliation processes: 1) the accuracy of the medication
reconciliation of the pre‐admission list to current orders and discharge orders, 2) the documentation of rationale for intended
medication discrepancies, 3) the incidence of unintended medication discrepancies, 4) the provision and assessment of
patient/caregiver medication education, and 5) the timeliness of provision of the reconciled discharge medication list to the
subsequent provider.
Instructions:
Using the criteria below, audit 5‐10 medical records of patients discharged from your facility on any anticoagulant or
hypoglycemic drug.
Answer Y or N to the following audit criteria questions using data elements found in the patient’s medical record.
For questions contact: Anne Myrka, anne.myrka@area‐i.hcqis.org
Please use additional copies of this form if your audit exceeds 5 patient records.
Please FAX this completed form to 518‐426‐3418 to Anne (main phone:518‐426‐3300)
Medication Reconciliation Audit Criteria ‐ DISCHARGE
Pt. 1
Pt. 2
Pt. 3
Pt. 4
Pt. 5
Y/N
Y/N
Y/N
Y/N
Y/N
Was the original home medication list (pre‐admission list)
reconciled with current orders and discharge orders?
Was there is a 1:1 match for every medication on the home
medication list (pre‐admission list) to the current orders and to
the discharge orders? (all elements for all drugs must match
for Yes)
For medications without a 1:1 match, was a rationale for the
discrepancy documented? If No, please complete the
Medication Discrepancy Tool (MDT‐ see below) (use one MDT
for each applicable patient record).
Did the reconciled medication list include the medication
name, dose, route and frequency for each medication? (all
elements for all drugs must be present for Yes)
Did the reconciled medication list include the date and time of
last dose given for each medication? (must be present for all
drugs for Yes)
Did the reconciled medication list include the date and time of
the next dose due for each medication? (must be present for
all drugs for Yes)
Did the final reconciled medication list for discharge indicate
whether medications should be stopped, started, or
continued?
Was patient/caregiver education provided?
Was patient/caregiver understanding of education assessed
and documented? (both elements must exist for Yes)
Was the final reconciled medication list communicated to
subsequent providers within 24 hours of discharge?
“Original Home medications list” and “pre‐admission list” refer to medications the patient was taking where they lived prior to admission to your facility and
includes lists provided by skilled nursing facilities, assisted living facilities, adult homes, home healthcare agencies, primary care, etc.
This material was prepared by the Atlantic Quality Innovation Network/IPRO, the Medicare Quality Innovation Network Quality Improvement Organization for
New York State, South Carolina, and the District of Columbia, under contract with the Centers for Medicare & Medicaid Services (CMS), an agency of the U.S.
Department of Health and Human Services. The contents do not necessarily reflect CMS policy. 11SOW‐AQINNY‐TskC.3‐15‐28
ADVERTISEMENT
1 votes
 1
1 2
2








